The expert spoke about modern approaches to the treatment of patients with osteochondrosis of the cervical spine

Alexey Peleganchuk, head of the neuroorthopedic department, orthopedic traumatologist, neurosurgeon, dr. , talked about what technologies are available to doctors today to help such patients.
What disease do patients usually call "cervical chondrosis"? What is the correct diagnosis?
– Actually, "cervical chondrosis" is jargon; the disease is correctly called "osteochondrosis of the cervical spine". This term is used by doctors in the post-Soviet space and corresponds to the current ICD (International Classification of Diseases), according to which we work. However, in most countries such a disease does not exist, they call it a "degenerative-dystrophic disease". When making a diagnosis, we indicate "osteochondrosis of the cervical spine" and then decipher which segments of the spinal movement are affected.
People most often associate this disease with pain in the cervical spine. Is this the main and/or only symptom?
- The most common reason such patients go to a neurologist is pain. We can say that the main clinical manifestation of degenerative pathology - osteochondrosis of the cervical spine, in this case is pain. In addition, even more dangerous manifestations of common degenerative pathologies are weakness of the upper extremities (perhaps in the lower extremities) and impaired sensitivity - numbness.
Can headaches and tinnitus occur with osteochondrosis of the cervical spine?
- These are uncharacteristic complaints for cervical osteochondrosis, but sometimes they happen. If such a patient comes, then this is first of all the reason for ordering an MRI of the brain in order to rule out any organic changes. If the patient has done this, is not amenable to conservative treatment and there is a substrate in the form of disc protrusions, which is extremely rare, but can reflexively cause these phenomena, then there is an option to help this patient, but the effectiveness will be significantly lower than the classic treatment of pain in the cervical spine.
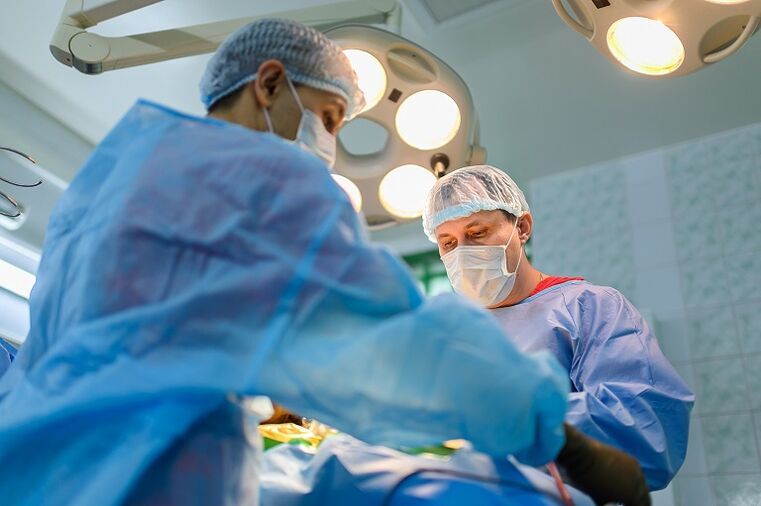
What are the causes of pain and what treatment options are available for such patients today?
– Three groups of patients can be distinguished. The first group are reflex pain syndromes, the second group are radicular syndromes, myelopathy - lesions of the spinal cord itself, as in severe stenosis, and the third are extremely rare patients, but the most complex, those who suffer the most are patients with neuropathy.
Reflex pain syndrome can spread locally to the cervical region, and it can radiate to the shoulder girdle and upper limbs. But the peculiarity of this pain syndrome is that the nerve tissue - that is, the spinal cord and its roots - is without compression (without compression).
Accordingly, in this case, if we think about the possibility of surgical treatment, then these are outpatient methods - for example, blockades. More invasive procedures include radiofrequency denervation and cold plasma coblation of the intervertebral discs - a hardware puncture procedure performed without incisions.
The goal is to remove the pain syndrome or significantly reduce its intensity, and free the patient from the need for analgesics.
Another group of patients are patients with hernias. Hernias in the cervical spine can cause root compression, and if conservative treatment methods are ineffective, surgery is resorted to. The purpose of the operation is to perform decompression, i. e. remove the hernia, that is, the root of the spinal cord will be free and the pain syndrome will go away.
In large hernias, there are also conduction disorders: in addition to compression of the spinal cord root, the spinal cord itself can be compressed (compressed). Then the person experiences more severe clinical manifestations in the form of tetraparesis, i. e. weakness of both the upper and lower extremities. In that case, it is necessary to decompress - create spare spaces for the spinal cord so that it can recover another time. It is important to understand that the operation does not restore the spinal cord and nerve, but rather creates conditions, i. e. reserve spaces.
In addition to hernias, there are also circular stenoses. They develop due to complex problems that arise in the cervical spine, which leads to a circular narrowing of the canal.
These are difficult patients who sometimes remain ill for years, and, unfortunately, they are most often admitted with a severe neurological deficit and often require a two-stage operation.
Another group of patients are people with neuropathic pain syndrome. In this case, patients, in the absence of stenosis, have neuropathy (the nerve itself hurts). Then help is provided using neuromodulation (neurostimulation). It involves the installation of special epidural electrodes on the posterior structures of the spinal cord. This is a special device - you could say, like physical therapy, that you always have with you: you can turn it on and increase the power to reduce pain. And it helps well even in very difficult cases.
All these technologies are available to patients, there are various sources of funding, including compulsory health insurance and quotas for high-tech medical care.
Can osteochondrosis be cured?
- The disease itself, osteochondrosis, cannot be cured. What can be done? Let's say a conditional patient: osteochondrosis of the cervical spine, with a predominant lesion at the level of the C6 - C7 vertebra, degenerative stenosis at this level and with compression of the C7 spinal cord root on the right.
During the operation, it is possible to remove the stenosis, remove the hernia or decompress the root of the spinal cord if the spinal cord itself is compressed. But the first four words of the diagnosis (osteochondrosis of the cervical spine) will remain for life, because it is incurable. Surgeons influence the substrate of this clinic, and the substrate of the clinic is, for example, a hernia that led to stenosis.
How is the treatment strategy determined?
- There is such a concept - clinical-morphological correspondence. The doctor must look at the patient from all sides - perform an orthopedic examination, a neurological examination, collect anamnesis, complaints - and connect this data with studies.
Screening studies for osteochondrosis of the cervical spine are MRI, unless this study is contraindicated for the patient for one reason or another. If necessary, MSCT is also prescribed to determine the tactics of the operation.
However, not every hernia described in an MRI requires surgery. A hernia alone is not a reason for surgery. The specialist must determine how much it causes compression, etc. and decide on the advisability of surgery.
At what age do such problems most often occur?
- The average age of our patients is over forty years old, but it happens that even young people require surgical intervention if their degenerative cascade started early, which led to the formation of a substrate in the form of a hernia. In this case, the first step is conservative treatment, and if there is no effect, then the only option is surgery.
What are the risk factors?
- We don't live in India, and our compatriots don't wear anything on their heads. Therefore, it is not necessary to say that work or habits lead to premature wear and tear and the creation of these formations.
The main risk factor is genetic. This applies not only to the cervical, but also to the thoracic and lumbar parts - this is the weakness of the tissue of the fibrous ring. And other risk factors - in the form of excess body weight, extreme work - are more reflected in the lumbar area.
Is it possible to somehow prevent it?
- Prevention is, above all, exercise therapy, so that the muscles are toned, the muscles work properly and there are no cramps. The fact is that when a degenerative process develops, and it can develop both in the discs and in the joints of the spine, it leads to muscle spasms, and the person feels pain. Therefore, massage, acupuncture, etc. good for reflex pain syndrome.
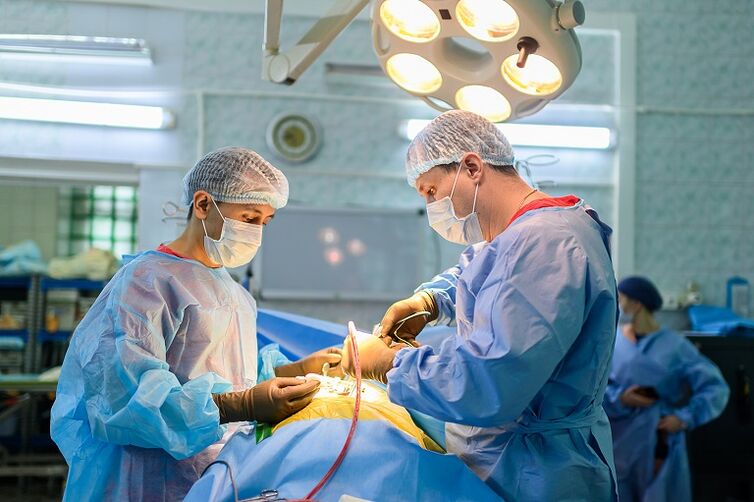
What determines the effectiveness of treatment?
- It is important to consult a neurologist in a timely manner if there is a problem: pain in the cervical spine that spreads to the upper limbs, numbness and weakness in the hands, reduced strength. Very serious pathologies are circular stenosis, when weakness in the lower extremities is added, when the spinal cord is already affected.
It happens that people last for years and think it's just "age-related". But every year they get worse, and as a result, the disease leads to the fact that they have limitations in movement - they can only walk a few meters.
The specialist will assess the degree of danger and, if necessary, refer to additional research methods and, if necessary, to a vertebrologist who deals with the surgical treatment of spine pathology. The purpose of the consultation is to determine the need for surgical intervention. If there is no need for surgery, then the neurologist is already dealing with conservative treatment. If surgical treatment is required, an operation is performed, after which the patient is sent to a neurologist for rehabilitation.
The goal of conservative treatment is to achieve very long periods of remission and minimize the frequency of exacerbations, both in terms of duration and frequency. This also applies to puncture treatment methods. But if there are already gross changes in the form of a hernia and compression of the spinal cord root, then conservative treatment may not work.
At the same time, the operation must be timely. The purpose of the operation is to save nerve tissue, either the spinal cord or its roots. If a person is sick for years, it leads to myelopathy - changes in the spinal cord itself, which then, even with excellent surgery, may not recover, or radiculopathy - damage to the roots of the spinal cord.
If the operation is performed on time, according to the standards, then there is a high probability of restoring both the roots of the spinal cord and the spinal cord itself, and the person will feel practically healthy after rehabilitation.
With advanced pathology, the effectiveness of surgical intervention decreases. In the case of persistent neurological disorders, surgery may not lead to noticeable improvement, because the spinal cord or root itself has already died by the time of surgery.
Every patient with one or another variant of the pathology needs a personal consultation with a specialist. At the same time, most patients with cervical osteochondrosis can be helped without surgery, using complex conservative treatment methods.
























